Making a Fetus Grow
Published on 22 October 2013 in Food, health and wellbeing
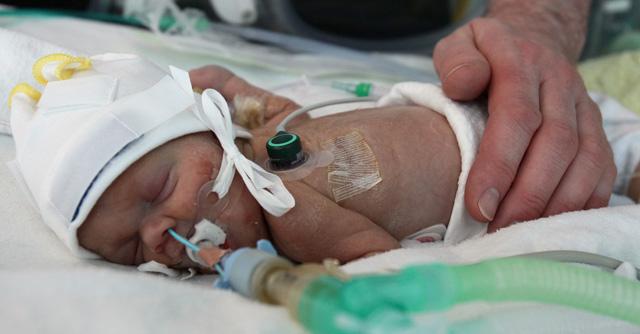
Fetal growth restriction, leading to low birth weight, complicates ~8% of pregnancies in the UK. It is a major cause of perinatal mortality and surviving babies experience a plethora of health complications throughout their life-course. The gravity of these complications is dependent on weight and gestational age at delivery.
Currently there is no effective treatment once severe growth restriction has been diagnosed at the mid-pregnancy ultrasound scan. Thus, there is a requirement to evaluate therapies to improve fetal growth as even a small increase in growth is likely to extend gestation and improve pregnancy outcome with major health, social and economic benefits.
Key Challenges
Premature delivery and low birth weight are particularly common in young still-growing adolescent girls. In the mid 1990s a unique adolescent sheep model was developed at the Rowett Institute to investigate the links between nutrition and fetal growth in this at risk group.
Early studies revealed that inadequate placental development was central to poor pregnancy outcome in growing adolescents. Moreover by mid-pregnancy, placental blood flows were reduced, limiting fetal nutrient supply, and directly leading to a slowing of fetal growth in the final third of pregnancy. Premature delivery of small lambs with a range of neonatal complications followed.
As well as mirroring the key features of poor pregnancy outcome in young adolescents, this sheep model replicates the major uteroplacental defects associated with human fetal growth restriction irrespective of maternal age. This makes it a valuable tool for evaluating therapies aimed at improving the nutrient supply to the fetus and hence its growth.
Key Benefits
It is well established that low uterine blood flow limits fuel supply to the developing fetus. An innovative approach to improving blood flow has been developed by collaborators at UCL. This involves locally targeting the uteroplacental circulation using adenoviruses (Ad) encoding vascular endothelial growth factor (VEGF).
VEGF plays a significant role in blood vessel development and function, and, when the gene therapy is applied to normal sheep pregnancies, uterine blood flow is enhanced for up to four weeks. However before progressing to the clinic, proof of concept was required that the gene therapy would enhance growth in severely compromised pregnancies.
This has now been obtained in our sheep model.
Ad.VEGF treatment in mid-pregnancy has increased ultrasound measurements of fetal abdominal circumference, the strongest marker of fetal growth in humans, at 3 and 4 weeks after treatment.
The amount of fetuses characterised as severely growth restricted was decreased and birth weight was increased by 20%.
As well as effectively improving fetal growth velocity, both pregnancy and term studies have shown that the gene therapy treatment is completely safe for both mother and fetus at the time of its application, at delivery and during the first three months of postnatal life.
Our collaborators have since secured funding from an EU FP7 grant to complete full reproductive toxicology, a bioethical study, and a first in-woman phase 1/2a safety/efficacy trial - see EVERREST.
If successful this research will reduce the number of stillbirths and neonatal deaths and improve long term outcomes in pregnancies affected by severe fetal growth restriction.
Comments or Questions
Related Websites
Our Partners
This work was funded by the Scottish Government, the Wellcome Trust and Wellbeing for Women. The gene therapy studies were carried out in collaboration with Drs. Anna David and David Carr, University College London.
Find Out More
Contact Dr Jacqueline Wallace via the details below.Author
Dr Jacqueline Wallace Jacqueline.Wallace@abdn.ac.uk







